Percutaneous laser disc decompression (PLDD) is a type of surgery in which a laser probe is inserted into the intervertebral disc space and laser energy is applied to achieve decompression and neuromodulation, thereby relieving the pain. It is performed under local anesthesia. Via a specially designed laser, with a coefficient of absorbing energy adjusted for soft discus tissue, a specific amount of heat is sent to achieve the evaporation of the water from the disc without additional thermal damage, thus achieving decompression and creation of a stable intradiscal scar that will prevent herniation from reoccurring. Given the above, it is important for the patient to understand that this is an indirect method of reducing intradiscal pressure, creating space to pull the disc bulge towards the center of the disc.
If you suffer from agonizing back or neck pain as a result of a herniated disc, PLDD (Percutaneous Laser Disc Decompression) offers quick relief without the need for classic open surgery.
Approved by the FDA (The United States Food and Drug Administration) and recognized by the AMA (American Medical Association), PLDD is a minimally invasive laser treatment performed on an outpatient basis using only local anesthesia. During the procedure, a laser beam vaporizes a tiny portion of the disc, decompressing it. Patients typically get off the table and go home. There is no hospital stay, no long recovery period, and PLDD costs many thousands of dollars less than traditional surgery.
PLDD is a minimally invasive medical procedure developed by Dr. Daniel S. J. Choy in 1986 that uses a laser beam to treat back and neck pain caused by a herniated disc. A herniated disc is like a balloon with a weak spot. Inflating it will cause a bulge (herniation). Pain results from the bulge pressing against nerves in the spinal column.
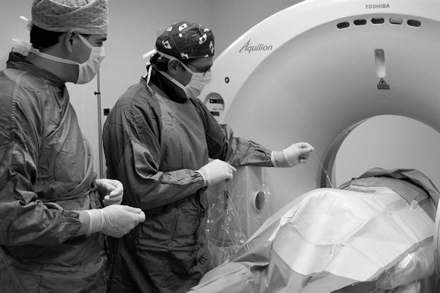
PLDD treatment is performed on an outpatient basis using only local anesthesia. During the procedure, a thin needle is inserted into the herniated disc under X-ray guidance. An optical fiber is inserted through the needle and laser energy is sent through the fiber, vaporizing a tiny portion of the disc nucleus. This creates a partial vacuum which draws the herniation away from the nerve root, thereby relieving the pain. The effect is usually immediate.
Patients get off the table with just a small adhesive bandage and return home for 24 hours of bed rest. Then patients begin progressive ambulation, walking up to a mile. Most return to work in four to five days.
Since only a thin needle is used, there is no cutting and no scarring. Since only a tiny amount of disc is vaporized, there is no subsequent spinal instability. PLDD is different from open lumbar disc surgery because there is no damage to the back muscle, no bone removal or large skin incision. Most of the complications that may occur with open surgery are eliminated with the PLDD procedure.
Who should consider PLDD?
This procedure is specifically designed for patients with disc problems accompanied by the following:
- severe leg, arm, neck or lower back pain
- pain that has not responded to six weeks of conservative treatment – rest, meds or physical therapy
- herniated lumbar discs confirmed by X-ray studies that may include one or more of the following: Magnetic Resonance Imaging (MRI), CAT scanning, myelography, discography.
Description and procedure
The withdrawal of symptoms (pain) manifests itself momentarily or in the next 2-10 weeks and depends on the structure of the disc. During this period, there are periods of withdrawal and onset of pain, new and old symptoms that can be alleviated by classic pharmacological pain therapy. Precisely for this reason, it is necessary to come back for a checkup after 2-3 months when the result is analyzed.
The surgery is performed under roentgen control and requires very rigorous precautions due to the cumulative effect of X-ray radiation on the surgeon while the patient is exempt from risk. The surgery lasts between 30 and 45 minutes and the patient can be discharged after 2 to 3 hours of stay in our polyclinic. International and our statistics predict: healing in 85% of cases; in 4-5% of cases in the first 5 years, hernia recurrences are possible. In 0.1% of cases, there is possibility of infection (regardless of the antibiotic therapy carried out in the 2 days after surgery). In this case, it is necessary to carry out antibiotic therapy for several weeks and rest. In cases of recurrent hernias after classic surgery, PLDD gives statistically worse results (approximately 70% compared to 85%). The reason for this is the scar tissue created by the classic procedure and the weakening of the spine. In 15% of cases in patients where the result is missing, it is always possible to perform minimally invasive, endoscopic or METRx surgery. In 10% of cases, it is not possible to place the probe in the disc, and this can only be checked during surgery.
After surgery, the patient must rest for 15-30 days and gradually return to daily activities. The patient must wear a lumbar brace for a period of 15 to 30 days and must follow the recommendations. PLDD does not guarantee that the condition of the herniated disc cannot worsen with time (week or years) after the surgery, but not because of the effect of the operation itself, but usually because of the patient’s activity after the postoperative course. Each patient is an individual case and therefore it is important to follow the written and verbal instructions that you receive from our doctors.
Unlike classic surgery, PLDD is a painless operation with no large surgical incision, it is performed under local anesthesia, there is no blood loss during the operation and no damage to the muscles, which are the main factors in the stability of the spine. After this surgery, in most cases, spa treatment is not necessary, and patients quickly return to their daily activities and work.