A bulging disc in the neck or back should not be confused with a herniated disc. Although they may have similar symptoms a herniated disc happens when the inner material of the disc seeps through a crack in its outer shell.
A bulging disc is usually a clear sign that there are problems in the surrounding areas of the spine. The problems may be caused by increased pressure being placed on the spinal disc, or by the disc weakening from degeneration. A bulging disc in the neck or back can be one of the causes of spinal stenosis, sciatica, or a pinched nerve.
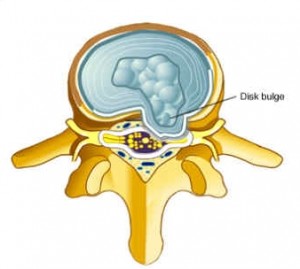
Symptoms
Most people who show signs of a bulging disc will feel pain in the area of the bulge. Numbness, tingling, and waves of pain felt along the nerve pathway into the arms or legs are also bulging disc symptoms that you may feel. Bulging disc symptoms will usually only be felt when they flare up from activity that puts pressure on a nearby nerve. Where the damaged disc is located will determine what other areas of the body are affected.
Bulging Disc in Neck Symptoms
- Neck pain
- Pain in the shoulder, arms, and/or hands
- Numbness or tingling felt in the arms, hands, or fingers
- Muscle weakness if left untreated for too long
Bulging Disc in Back Symptoms
- Lower back pain
- Pain in the buttocks, legs, and/or feet
- Numbness or tingling in the legs, feet, or toes
- Muscle weakness if left untreated for too long
As you can see bulging disc in neck symptoms are quite similar to the symptoms of a bulging disc in the back. The only difference being that a bulging disc in the neck will affect the nerves that reach out into your arms, while a bulging disc in the lower back will affect the nerves that run down your legs.
Lumbar bulges (bulging discs in the lower back) are more common than bulging discs in the neck. 90% of patients with lumbar bulges will actually experience bulging disc symptoms.
What non-surgical bulging disc treatment options are available to me?
Conservative treatment of a bulging disc usually begins with rest and anti-inflammatory medicine. If your bulging disc does not improve, physical therapy and activity modification is usually the next step for bulging disc treatment.
Heat and cold is often added to a bulging disc treatment plan to help encourage healing. Cold is usually used for the first 48 – 72 hours to reduce the inflammation in the injured area. Heat would then be rotated in to encourage blood flow and healing to the affected area.
If your symptoms are severe and threaten to cause permanent damage to your spine or its surrounding structures, surgery may be required before conservative methods are attempted.
We use advanced diagnostic tools and procedures to develop a treatment program tailored to your specific condition. Several factors such as the location of your bulging disc, the severity of your symptoms, and how long you’ve been experiencing them will all be considered when developing your bulging disc treatment program.
When should I consider bulging disc surgery?
After 4-6 weeks of treatment have passed and you feel little to no relief from your symptoms, bulging disc surgery may be considered. Having a bulging disc operation, however, is a last resort and is rarely required.
If your bulging disc is causing numbness or muscle weakness that affects your walking, or you are having problems with bowel or bladder function, surgery for a bulging disc is usually considered a priority.
What bulging disc surgery options are available to me?
Open Back Surgery
Traditionally, bulging discs are treated with an open back procedure, meaning the surgeon makes a large incision into the skin and cuts muscle and surrounding tissue to gain access to the problematic disc. This traditional surgical option is invasive, requires overnight hospitalization, general anesthesia, and requires a lengthy recovery coupled with strong pain medication.
Endoscopic Surgery
Fortunately, you have a second option, endoscopic spine surgery. Thanks to the advancement of surgical technology, bulged disc surgery can be performed using endoscopic procedures, meaning the surgeon makes a small incision to insert special surgical tools. During an endoscopic bulging disc operation, the surgeon uses a tiny camera to visualize and gain access to your damaged disc. This minimally invasive new approach offers shorter recovery, easier rehabilitation, and much higher success rate than open back or neck surgery. A local anesthetic is all that is usually required for this bulging disc operation.
Endoscopic Discectomy
An endoscopic discectomy is performed to remove a portion of a damaged disc that is causing pain and other symptoms. Because of how the surgery is performed there is no need to remove bone, cause muscle damage, or make large incisions in the skin. With the use of x-ray imaging and video magnification we are able to guide an endoscopic probe into the damaged disc space and use special tools to remove the debris.
Endoscopic Foraminotomy
An endoscopic foraminotomy is performed to relieve pressure caused by other conditions such as bone spurs, disc bulges, disc herniations, scar tissue, or excessive ligament growth. This is a minimally invasive procedure that requires little recovery time allowing our patients to return to their normal daily activities quicker.
Percutaneous Laser Disc Decompression
PLDD is a minimally invasive laser treatment performed on an outpatient basis using only local anesthesia. During the procedure, a laser beam vaporizes a tiny portion of the disc, decompressing it. Patients typically get off the table and go home. There is no hospital stay, no long recovery period, and PLDD costs many thousands of dollars less than surgery.